9th of December 2022
Orthopaedic visit - 5 December to 9 December 2022.
Visit summary
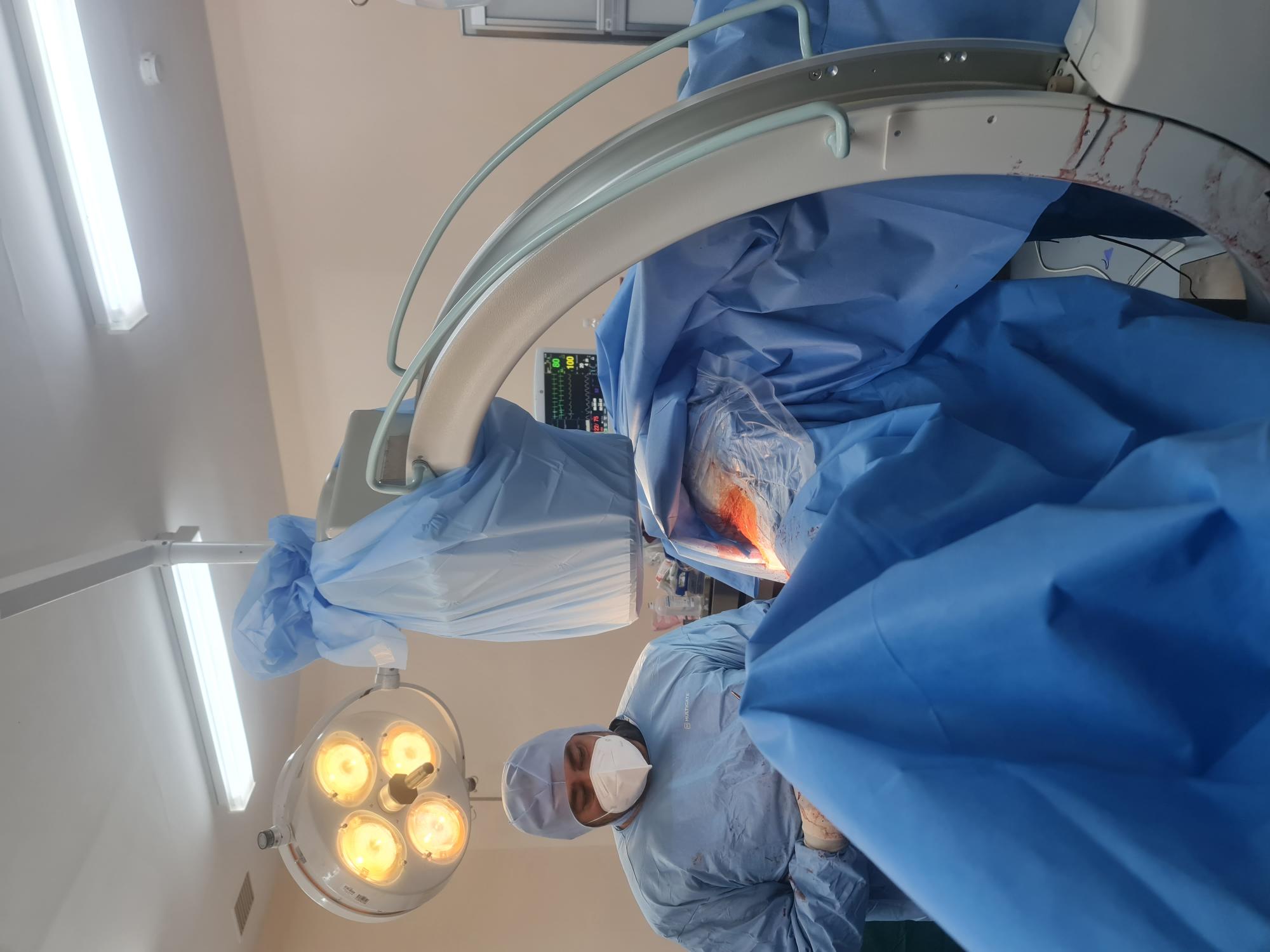
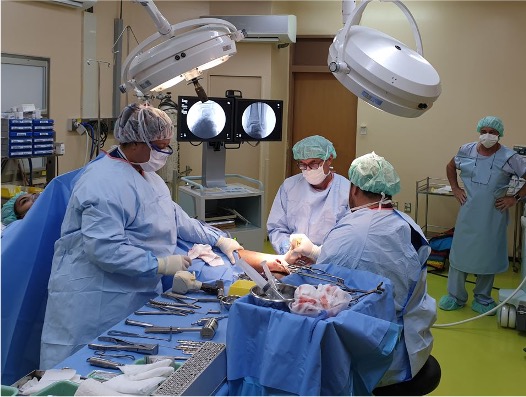
I arrived in Tonga Monday morning 5 December on an early flight from New Zealand. This enabled me to commence an Out-Patient clinic soon after mid-day, reviewing some 30 patients during the afternoon session, with the resident surgical team. This was followed by a ward round assessing five inpatients that required surgery that we planned for later in the week.
During the week a young Doctor of Tongan descent, currently working in Tauranga hospital, Dr Charlotte Fakahau, who has an interest in specializing in Orthopaedic Surgery, worked alongside me. Despite mainly observing Charlotte was a great help in sorting out the equipment for me.
On Tuesday the operating was focused on cases that did not require the use of extensive orthopaedic equipment. In between cases I was able to prepare equipment for the following operating days so that the Trauma table could be utilised.
Wednesday, however, was marred by a burst water pipe in the Central Sterile Supply department that caused extensive flooding in theatre and other parts of the hospital. According to Dr Tangi this was the first time in his memory that this had happened at Vaiola hospital. Operative procedures were cancelled because of the risk of electrical malfunction due to the dampness in the operating theatres.
Thursday and Friday morning proved to be more productive with challenging operative cases as listed below, utilizing the trauma table, and newly acquired equipment.
I flew back to New Zealand on an afternoon flight that left at 2.30 pm, an hour late, causing me to miss my connecting flight to Whanganui.
Clinical work
Outpatients
Monday 5 December 2022
1. Outpatient dept – Vaiola hospital.
Reviewed 30 patients with Drs Alamea Aholelei, Tevita Tu’ungafasi and Selesia Fifita from 12.30pm to 4.30 pm.
Refer to Appendix 1 for cases seen at the clinic and during the week in the Theatre suite.
Theatre
Tuesday 6 December 2022
1. SK Male 8 years Laceration dorsum of finger through the extensor hood and proximal phalanx. ORIF and fixation of the proximal phalangeal fracture index finger. Surgeon Dr Tevita Tu’ungafasi, Assistant Mr John van Dalen.
2. OM Male 28 years Open fractures of 2nd and middle metacarpal and partially amputated middle finger right hand. Amputation of middle finger and washout of wounds right hand. Surgeon Dr Tevita Tu’ungafasi, Assistant Mr John van Dalen.
3. PA Male 18 years. Fungating wound left hindfoot. Excision of fungating wound left hindfoot and closure with partial subcuticular tension suture. Surgeon Dr Alamea Aholelei Assistant Mr John van Dalen
4. MV Male 27 years. Neglected rupture of the ligamentum patella right knee joint. Reconstruction of old ruptured ligamentum patella right knee joint. Surgeon Mr John van Dalen Assistants Dr Alamea Aholelei and Dr Tevita Tu’ungafasi.
5. HS Male 62 years. Post traumatic osteophyte left ankle joint. Excision of anterior osteophyte left ankle joint. Surgeon Mr John van Dalen, Assistant Dr Tevita Tu’ungafasi.
In addition to the above operations considerable time was spent sorting out equipment from India for cases the following day.
Wednesday 7 December
Surgery was cancelled due to flooding of the theatre area.
I reviewed a male patient with cubital tunnel syndrome effecting his left elbow joint and will review him at my next visit in March.
I arranged a referral for a 43-year-old woman to the Sarcoma Middlemore team in New Zealand for advice on further management of a large cancerous soft tissue lesion on her left knee joint.
Again, considerable time was spent checking the equipment from India ready for sterilizing for operative procedures to be undertaken on Thursday and Friday.
A surgical ward round was also arranged reviewing patients that had been operated on the previous day. I also reviewed the patients planned for surgery on Thursday and Friday.
Thursday 8 December
1. AV Female 63 years. Pathological non-union fracture right neck of femur. Right hemi arthroplasty right hip joint. Surgeon John van Dalen, Assistant Drs Tevita Tu’ungafasi and Alamea Aholelei.
2. SF Female 12 years. Acute on chronic significant SUFE right hip joint. ORIF for slipped upper femoral epiphysis right hip joint. Surgeon John van Dalen. Assistant Dr Alamea Aholei. Trauma table was used for this case.
3. FL Male 22 years. Hypertrophic non-union left Neck of Femur. ORIF with dynamic hip screw and plate left hip joint. Surgeon John van Dalen. Assistant Dr Alamea Aholelei. Trauma table was used for this case.
Refer to Appendix 2 for photos of trauma table.
Friday 9 December
1. MF Male 17 years. Displaced mid shaft fracture right Tibia. Interlocking nailing of right Tibial shaft fracture. Surgeon Mr John van Dalen, Assistant Dr Tevita Tu’ungafasi and Alamea Aholelei.
Refer to Appendix 3 for photos
________________________________________________________________
Planning
I was able to plan my three visits with Dr Tangi for 2022, which have tentatively been set for:
2. March 27 – 31
3. August 28 – September 1
4. November 20 - 24.
I am hoping a colleague will come with me on one of my visits, so that in the future it may allow for more frequent specialist visits.
Equipment
On this trip I was able to bring a vital bracket and an extra screw for the trauma table that were missing as identified on my September visit. Testing of the Trauma table proved to be fine, allowing me to have the confidence to use it for operative cases for this visit.
In addition, a complete external fixator set, donated by Whanganui hospital, was added to the equipment range. I was also able to bring three Pulse lavage sets donated by Stryker which the Surgical team are very thankful for. They not only use them for contaminated wounds in the upper and lower limbs but also in infected abdominal wounds and abscesses.
This visit highlighted some deficiencies in the current equipment range that will need to be updated by my next visit in March 2023:
· Metre long beaded guide wires for intramedullary nailing. X3
· Guide wire hand holding clamp x 1
· An updated intramedullary reaming set, to allow for adequate insertion of intramedullary nails. The current reamers are old and in fact during the tibial case a reamer failed altogether.
· Special pointed 3 and 4 mm drills bits for intramedullary interlocking drill holes X3
· Sterile drapes to be used for the trauma table cases. X20
· 6.5 cannulated screws 50mm, 55mm, 60 mm and 65mm lengths X3 each
· 110 mm Richards screws X2
· Supports for the theatre table to enable patients to be positioned in the lateral decubitus position eg Hemiarthroplasty.
· Pulse lavages – Donated by Stryker
Replacements required:
· 10 x 320 Tibial nail
· 47 mm diametre Austin Moores prothesis
· 105 mm Richards screw
· 135 degree four hole plate
Other than that, the equipment now available is near complete and should serve us well for the next few years. As the surgeons become more confident with the use of this equipment, more of the equipment will obviously be used but I don’t envisage a shortfall for at least a couple years.
Trauma table
With respect to the trauma table, I am looking at the option of securing another table from New Zealand as some of these tables will be coming up to their used by date. If a table is secured, then it would be serviced before being transported to Tonga. This would overcome the expense of yearly maintenance of the current trauma table in Tonga, which is a costly exercise and overcome the problem if a table were to fail, then there would be a backup. I have spoken to Dr Tangi about this, and he is agreeable.
I will speak to Victoria Nussbaume of Gettinge the company responsible for servicing the trauma table and seek advice as to whether this is an option to consider.
________________________________________________________________
Conclusion
Overall, despite the setback on Wednesday this visit proved to be extremely valuable. The positives were that the equipment procured from India and the availability of the trauma table allowed cases to be done that otherwise could not have been. In addition, the local surgeons were involved, and were able to learn new orthopaedic surgical techniques. It won’t for a year or so before they become confident using the trauma table with the new equipment, but at least this visit has been a successful start.
Dr Tevita Tu’ungafasi is still committed to coming to New Zealand to work in Whanganui hospital in 2024 and will be resitting the English medical examination early next year.
In due time I firmly believe the goal of upgrading Orthopaedic Surgical services in Tonga is attainable. This would not have been possible without the generous support from NZ Aid, Rotary International, Rotary clubs of New Zealand and multiple private donations.
John van Dalen FRACS
Orthopaedic Surgeon
Whanganui, New Zealand